(What will be mentioned in this article is for advice and is not a substitute for consulting a doctor)
Cancer Research Breakthroughs 2026: New Pancreatic Cancer Treatments, AI Detection, and Future of Oncology
Key Takeaways
A new KRAS-targeting drug, daraxonrasib, is showing major survival improvements in pancreatic cancer.
Clinical trials suggest survival time may nearly double compared to standard chemotherapy.
Artificial intelligence is transforming early cancer detection and predicting disease spread with high accuracy.
advertisement
Introduction: A Rapidly Changing Landscape in Cancer Research
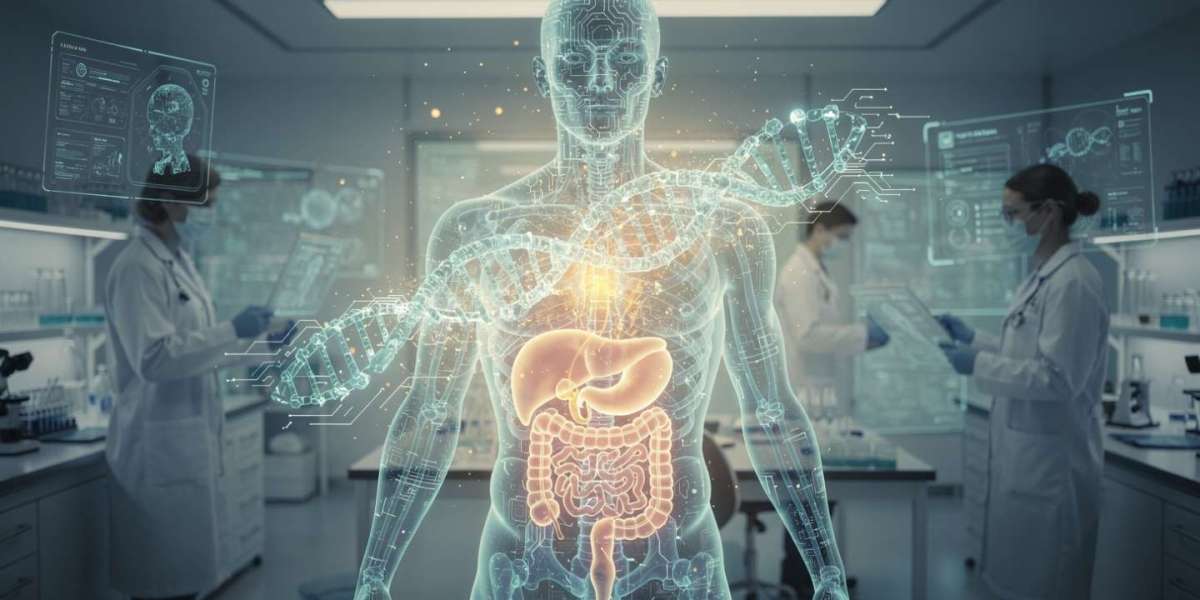
Cancer research is undergoing one of its most significant transformations in decades. Advances in targeted therapies, genetic medicine, and artificial intelligence are converging to reshape how cancers—especially pancreatic cancer—are detected and treated.
Recent clinical trials and emerging technologies are offering new hope in a disease long considered one of the most difficult to manage, with researchers now reporting meaningful improvements in survival and diagnosis accuracy.
1. KRAS-Targeted Therapy and the Breakthrough in Pancreatic Cancer Treatment
One of the most important developments in oncology is the targeting of a genetic mutation called KRAS, found in nearly 90% of pancreatic tumors. This mutation acts like a biological “on switch,” driving uncontrolled cancer cell growth.
For decades, KRAS was considered undruggable. However, recent clinical research has changed that perspective.
A new oral drug, daraxonrasib, is designed to bind to the mutated KRAS protein and block its cancer-driving signals. According to clinical trial data, patients receiving this therapy showed a median survival of 13.2 to 15.6 months, compared to 6.7 months with standard chemotherapy.
This represents nearly a doubling of survival time in some studies, a result described by oncologists as unprecedented in pancreatic cancer treatment.
Researchers also observed additional benefits:
Tumor shrinkage in roughly 29% of patients
Disease stabilization in over 90% of cases
Potential for improved quality of life compared to traditional chemotherapy
Experts emphasize that even a few extra months of survival in pancreatic cancer is clinically meaningful due to its aggressive nature and late diagnosis patterns.
2. Clinical Impact, Patient Experience, and the Future of Treatment Strategies
Pancreatic cancer remains extremely difficult to treat, largely because about 80% of patients are diagnosed at advanced or metastatic stages. At this point, treatment options are limited, and the five-year survival rate remains around 3%.
Traditional chemotherapy is still the standard treatment, but it affects both cancerous and healthy cells, often leading to strong side effects such as fatigue, nausea, and immune suppression.
In contrast, daraxonrasib represents a shift toward targeted therapy, which focuses specifically on cancer-driving mutations. Patients in trials have taken the drug orally, avoiding repeated IV chemotherapy sessions.
Doctors report that side effects do exist—such as rash, diarrhea, and fatigue—but are generally manageable with dose adjustments and supportive care.
Importantly, researchers are now exploring how this drug could be used:
As a first-line treatment
In combination with chemotherapy
Alongside emerging therapies such as mRNA-based cancer vaccines
Early experimental vaccine studies have shown promising results in preventing recurrence, although experts remain cautious about their broader effectiveness in advanced pancreatic cancer.
Despite these advances, specialists stress that daraxonrasib is not a cure—but rather a major step forward in extending life and improving treatment options.
3. Artificial Intelligence Transforming Cancer Detection and Prediction
Beyond drug development, artificial intelligence (AI) is emerging as a powerful force in cancer care.
In one documented case, an AI system used in breast cancer screening detected a tumor that was not visible to the human eye. This early identification allowed for faster diagnosis and successful treatment at an early stage. Research suggests AI can improve cancer detection accuracy by more than 10%, while still working alongside human specialists.
AI is also being used to better understand how cancer spreads through the body. Researchers developed a system called Mangrove Gene Signatures (MangroveGS), which analyzes genetic data from tumor cell groups.
Instead of focusing on single cells, the system studies how groups of cancer cells interact, helping predict:
Risk of metastasis
Likelihood of recurrence
Disease progression patterns
This AI model has demonstrated nearly 80% accuracy in predicting cancer spread in early studies.
Experts believe this technology could soon help doctors:
Identify high-risk patients earlier
Avoid overtreatment in low-risk cases
Personalize cancer therapies more effectively
Improve clinical trial design and efficiency
This represents a shift toward precision oncology, where treatment decisions are guided by both biology and machine intelligence.
Conclusion: A Turning Point in Cancer Research
Cancer treatment is moving into a new era defined by precision, intelligence, and personalization.
The development of KRAS-targeting drugs like daraxonrasib shows that even long-dismissed genetic mutations can now be successfully targeted, offering real improvements in survival for patients with pancreatic cancer. At the same time, artificial intelligence is expanding the boundaries of early detection and predictive medicine, making cancer care more proactive and data-driven.
While challenges remain—especially in early diagnosis and achieving long-term cures—the combination of targeted therapies and AI-driven insights represents a meaningful shift in oncology.
The future of cancer research is no longer defined only by hope, but increasingly by measurable progress, scientific innovation, and a growing ability to intervene earlier and more effectively in the course of disease.
Key Points
KRAS-targeting drug daraxonrasib significantly improves pancreatic cancer survival.
Clinical trials show survival can nearly double compared to chemotherapy.
AI improves early cancer detection and predicts metastasis with high accuracy.
Pancreatic cancer remains difficult due to late diagnosis and low survival rates.
The future of oncology is moving toward personalized and AI-assisted treatment.
advertisement
Frequently Asked Questions (FAQ)
1. What is daraxonrasib used for?
It is an experimental drug targeting KRAS mutations in pancreatic cancer.
2. Does daraxonrasib cure pancreatic cancer?
No, but it significantly improves survival and disease control in trials.
3. Why is KRAS important in cancer?
KRAS is a gene mutation that drives uncontrolled cancer cell growth in many tumors.
4. How does AI help in cancer detection?
AI analyzes medical images and genetic data to detect cancer earlier and more accurately.
5. Can AI predict cancer spread?
Yes, systems like MangroveGS can predict metastasis risk with about 80% accuracy.
6. Why is pancreatic cancer so deadly?
It is usually diagnosed late, spreads quickly, and has limited early symptoms or screening options.
Sources
- National Geographic – KRAS-targeting drug breakthrough and pancreatic cancer trials
https://www.nationalgeographic.com/health/article/pancreatic-cancer-kras-drug-daraxonrasib-trial-results - Baptist Health – Clinical trial results of daraxonrasib in pancreatic cancer
https://baptisthealth.net/baptist-health-news/experimental-pancreatic-cancer-drug-doubles-survival-time - LADbible – AI in cancer detection and metastasis prediction research
https://www.ladbible.com/news/health/ai-cancer-health-technology-screenings-treatments-990667-20260326
Disclaimer:
What is mentioned in this article is for advice and is not a substitute for consulting a doctor
Thank you !